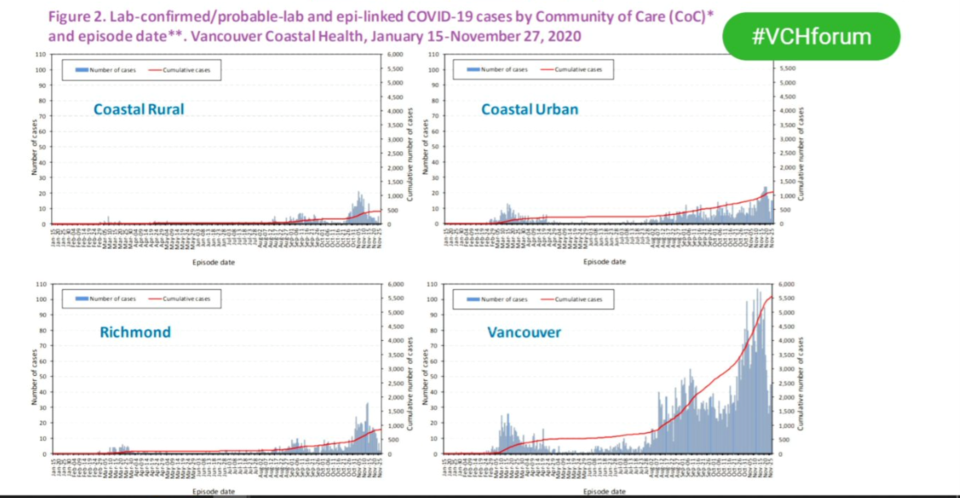
There were 48 confirmed cases of COVID-19 on the Lower Sunshine Coast between Jan. 15 and Nov. 27 – and at 148.5 per 100,000 people, the region has the lowest rate of COVID-19 of all local health areas in Vancouver Coastal Health (VCH).
The updated numbers were shared during a Nov. 30 virtual VCH board meeting, billed as an opportunity for community members to ask questions directly to officials, according to board chair Dr. Penny Ballem.
In October, the Sunshine Coast saw an increase of three cases and before that a jump from 14 in August to 26 in September.
Nov. 1 to 27 saw the total rise by 19 cases.
As for the other coastal rural areas, between January and the end of November there were 347 cases in Howe Sound, which includes Whistler and Sea-to-Sky, 41 in Powell River and five each in Central Coast and the Bella Coola Valley.
Apart from Whistler, Squamish and Powell River, no other municipality in the coastal rural areas has had more than 20 cases cumulatively since the start of the pandemic, and most have had less than five cases.
“The numbers are small,” said VCH chief medical health officer Dr. Patricia Daly.
She said the “vast majority” of cases in the second wave are linked to confirmed cases or clusters, and most transmission occurs in household settings and private gatherings.
Coastal rural communities, including the Sunshine Coast, have had six per cent of cases in VCH, while hospitalizations and ICU admissions are lower compared to the rest of the regions. Less than one per cent of deaths occurred in coastal rural areas, as well.
“That tells us that the cases in coastal rural communities have tended to be milder, with less impact on the populations with greatest risk of severe disease,” said Daly.
Most deaths in VCH, about 63 per cent, are associated with long-term care outbreaks. As of Dec. 1 there had been no outbreaks at Sunshine Coast facilities.
Daly said more detailed information would be coming to the BCCDC website.
Operations VP Karin Olson said in the second wave hospitals aren’t seeing as many COVID-19 admissions as during the first wave, and comparably fewer people are being admitted to ICUs.
Since the May 25 start of the surgical renewal program, about 93 per cent of the 120 surgeries and procedures postponed at Sechelt Hospital have been completed.
Vaccine
Daly also said at the meeting that VCH has been told by the federal government to expect the first shipments of vaccine to be delivered in early January.
Health Canada and provincial health officials have identified priority populations based on who is most at risk of severe disease, including residents and staff of long-term care facilities.
“We’re actively planning to administer the vaccine as soon as shipments arrive here,” she said, adding no vaccine will be administered until approved by Health Canada.
On Tuesday, Public Procurement Minister Anita Anand said Canada was one of the first countries to sign a deal with U.S.-based pharmaceutical firm Moderna – and that the company has confirmed it will be one of the first to receive doses of its vaccine.
Schools
After schools opened, Daly said, VCH and other health authorities did not see a rise in COVID-19 cases. “It’s evidence that the schools’ safety plans are very robust,” she said.
“Almost all” exposures occur outside of schools and “in very, very few cases has there been any transmission in the school setting,” said Daly. “We do believe that schools can safely continue to operate even as we’ve seen a rise in cases in more recent weeks.”
Restrictions
The rise in cases in October was accompanied by rules meant to address the most common types of transmission, including household and private gatherings without COVID safety plans. Daly said in VCH those restrictions have corresponded with “a further flattening of the curve within our region.” She said cases have been “holding steady” within the last few weeks and have not been rising.
In Plain Sight
At the start of the meeting, board chair Ballem described the day as “emotional and humbling” because of the release of former judge Mary Ellen Turpel-Lafond’s investigation into racism and discrimination within B.C.’s health-care system.
The report, titled In Plain Sight, found 84 per cent of Indigenous respondents reported discrimination in health care and provided 24 recommendations.
“I just want to say that racism and particularly anti-Indigenous racism in our organization is not acceptable. And we completely accept the findings in the report,” Ballem said. “We hear the truth telling and the courageous stories that thousands of people shared” over the course of the investigation.
– with files from the Canadian Press, Sean Eckford and Katie DeRosa